ClaimPath: Navigating Health Insurance Denials with AI
Health insurance claim denials are a major challenge for patients and providers. In 2023, $262 billion worth of claims were denied, with 65% of denials left unchallenged despite 90% of appeals succeeding. ClaimPath changes this by using AI to automate denial management, saving time and recovering lost revenue. Here's how it helps:
- Decodes Denials: Quickly identifies reasons for claim rejections using standardized codes.
- Automates Appeals: Drafts professional appeal letters tailored to specific insurers.
- Tracks Deadlines: Ensures appeals are submitted on time, avoiding missed opportunities.
- Prevents Errors: Analyzes patterns to reduce future denials by improving claim accuracy.
ClaimPath has cut denial-to-appeal timelines by 75%, reduced manual work by 90%, and saved organizations thousands in administrative costs. Patients and providers can now focus on care rather than red tape.
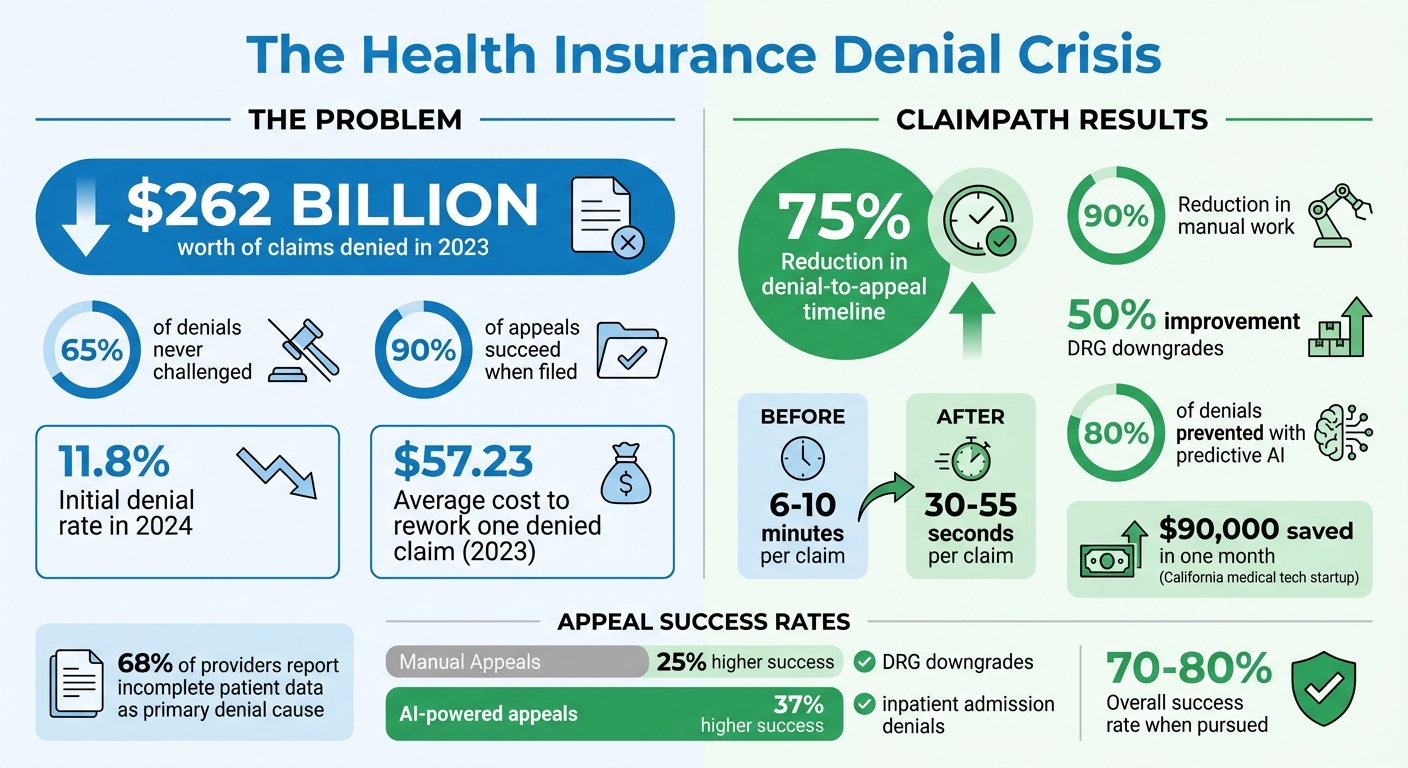
Health Insurance Claim Denials: Key Statistics and Impact 2023-2024
How patients are using AI to fight back against denied insurance claims
sbb-itb-8bb7924
How Health Insurance Denials Work
To challenge a denial successfully, it’s crucial to understand the claims process and the common reasons claims fail.
The Claim Lifecycle from Submission to Decision
The journey of a health insurance claim follows a structured path. It begins when your healthcare provider submits the claim to your insurer, typically through an API, electronic data interchange (EDI), or a web portal [5]. Before the claim even reaches the insurer, it passes through a clearinghouse, which performs pre-adjudication checks. These checks look for formatting errors, invalid subscriber IDs, or missing provider NPIs [6]. Claims with errors are rejected at this stage. If the claim passes, it moves into adjudication, where the insurer evaluates it against coverage rules, medical necessity guidelines, and contractual agreements. After this review, the insurer sends back an Electronic Remittance Advice (ERA) or Explanation of Benefits (EOB), detailing whether the claim is approved for payment, partially paid, or denied.
When a claim is denied (not to be confused with rejection), it means the insurer processed the claim but decided not to pay it. At this point, providers must determine whether to fix clerical issues by submitting a corrected claim or to formally appeal the decision, especially for disputes over medical necessity or policy interpretation.
Shockingly, up to 65% of denied claims are never corrected or appealed, even though 80% could be recovered if addressed properly and within the required timeframe [2][8]. This lack of follow-up contributes to many of the common issues behind claim denials, as outlined below.
Why Claims Get Denied
Several factors lead to claim denials, and understanding these can help reduce their occurrence:
-
Registration and Eligibility Issues:
Simple errors like a misspelled patient name, outdated insurance ID, or incorrect plan details can result in immediate denials. A staggering 68% of providers report that incomplete or inaccurate patient data collected during intake is a primary cause of denials. To combat this, OhioHealth introduced Experian Health's Patient Access Curator platform in 2025. This system cross-checks patient information against payer databases in real time, leading to a 42% drop in registration and eligibility-related denials, a 69% reduction in termed insurance denials, and a 63% decrease in incorrect payer denials [9]. -
Prior Authorization Failures:
Many claims are denied because required pre-approvals weren’t obtained, especially for specialty referrals or imaging services [9]. -
Coding Errors:
Mistakes like outdated codes, mismatched diagnoses, or incorrect billing can result in denials. Insurers use standardized Claim Adjustment Reason Codes (CARC) and Remittance Advice Remark Codes (RARC) on EOBs to explain the issue. For instance, CARC code CO-11 signals incorrect coding, while CO-15 indicates a missing authorization [1]. -
Medical Necessity Denials:
These arise when an insurer decides a procedure isn’t appropriate for the patient’s condition. Take the example of a pain management clinic in June 2025: A lumbar radiofrequency ablation (CPT 64635) was initially denied due to "lack of medical necessity." The provider had failed to include prior diagnostic block results in the documentation. By submitting the missing details and referencing the Medicare Local Coverage Determination (LCD) policy - which specifies at least 50% pain relief as a requirement - the clinic successfully overturned the denial and secured full payment [8].
| Common CARC Code | What It Means | Real-World Example |
|---|---|---|
| CO-11 | Incorrect coding | Diagnosis code does not match the billed service [1] |
| CO-15 | Missing authorization | MRI performed without prior approval [1] |
| CO-16 | Missing/incorrect info | Patient name misspelled or insurance ID mismatch [1] |
| CO-27 | Expired coverage | Service provided after the insurance plan ended [1] |
| CO-29 | Late submission | Claim filed beyond the 90-day deadline [1] |
| CO-50 | Medical necessity | Procedure labeled as cosmetic by the payer [1] |
| CO-252 | Additional documentation required | Operative notes needed to prove necessity for surgery [1] |
In 2023, the average cost to rework a single denied claim was $57.23 - a 30% increase from the previous year [9]. With the initial claim denial rate rising to 11.8% in 2024 [9], the financial and administrative strain on healthcare providers continues to grow. These challenges highlight the importance of adopting AI-driven tools to navigate the increasingly complex claims process.
ClaimPath: AI-Powered Denial Management
ClaimPath tackles the challenges of manual denial corrections head-on by introducing AI into the process. Instead of relying on staff to manually interpret denial codes, draft appeal letters, and track deadlines across multiple payer portals, the platform automates these tasks while maintaining the accuracy and compliance that healthcare providers demand. Operating around the clock, it handles everything from identifying initial denials to submitting final appeals.
This shift to AI-driven automation isn’t just about speeding things up - it’s about precision and prevention. Manual methods often fail to uncover the recurring patterns behind denials, leaving providers stuck in a cycle of rework. ClaimPath changes the game by analyzing denial data at scale, spotting systemic issues, and recommending solutions. Here's a closer look at how it works.
What ClaimPath Does
ClaimPath automates four major denial management tasks, saving significant time and effort:
- Denial parsing: The platform decodes CARC and RARC codes from EOB and ERA documents in seconds, pinpointing the reason for each denial without the need for manual review [6][12].
- EOB auditing: It cross-references denial reasons with clinical documentation and billing records to uncover root causes, such as mismatches between a physician's notes and the submitted CPT codes [11][13].
- Automatic appeals: ClaimPath generates payer-specific appeal letters, complete with clinical evidence and direct policy references like Medicare NCD/LCDs, eliminating the long hours spent drafting custom appeals [6].
- Deadline tracking: The system monitors claim statuses across payer portals, navigating complex security protocols to ensure no appeal deadlines are missed [2][5][6].
For example, in 2025, PathGroup implemented an automated pipeline connecting EHR and claim data across athenahealth and PathSys. This reduced claim processing times from 10 minutes to just 55 seconds, enabling roughly 300 automated resubmissions daily and clearing backlogs almost entirely [12]. Similarly, Smilist used AI agents to handle over 3,000 daily claim status checks, absorbing repetitive tasks that previously demanded multiple staff members [2].
How AI Identifies Denial Patterns and Prevents Repeat Problems
ClaimPath’s machine learning tools analyze trends across payers, service lines, and claim types to spot recurring problems [11][13]. For instance, if a specific insurer frequently denies claims for a particular CPT code due to missing documentation, the system flags this pattern and suggests adding the necessary documentation to future claims before submission.
With predictive risk modeling, ClaimPath examines historical data and payer-specific behavior to predict denial risks before claims are submitted, achieving up to 97% accuracy [5][13]. High-risk claims are flagged for manual review, allowing corrections to be made early. This proactive method prevents around 80% of denials that would otherwise require later intervention [5].
"The real value of AI in denial management isn't about replacing your staff - it's about removing the roadblocks that keep them from performing at their best." - Productive Edge [13]
Additionally, the system provides real-time feedback to clinical and billing teams, improving documentation accuracy from the start [10]. By linking denials to specific payer policies and coverage criteria, ClaimPath ensures preventive actions are based on concrete guidelines rather than guesswork [6]. This ongoing learning process turns denial management into a smarter, data-driven system that evolves with every claim processed. By addressing systemic challenges head-on, ClaimPath offers a proactive approach to eliminating recurring denial issues.
How to Use ClaimPath: A Step-by-Step Guide
ClaimPath works seamlessly with your current systems, requiring minimal effort to get started. It connects directly to the tools you already use, whether you're managing a high volume of claims or resolving a single denial. Here’s how to set it up and make the most of it.
Connecting Your Claim Data to ClaimPath
ClaimPath uses browser-based integration to connect with your existing software, eliminating the hassle of building complex APIs. The platform operates within your electronic health record (EHR), practice management system, and payer portals, mimicking the actions of a human team member. Providers can securely save their credentials, allowing the AI to handle multi-factor authentication and CAPTCHA challenges automatically. To train the AI on your workflow, upload 60 minutes of screen recordings.
For instance, in 2024, the dental RCM organization Smilist used this method and had their AI agents conducting over 3,000 daily claim status checks across payer portals - tasks that previously required several full-time staff members [2].
"Ventus stands out from the noise in the AI and automation market. Their approach allows them to ramp up quickly in the messy middle of RCM."
- Philip Toh, Co-founder & President, Smilist [2]
Policyholders can also link their health insurance accounts to sync claims and coverage details or upload images of medical bills, denial letters, and clinical notes for analysis. Additionally, ClaimPath integrates with tools like Slack, Microsoft Teams, and email to provide real-time updates. Start small by piloting one high-volume denial category, such as eligibility issues, to test the system before expanding to all payers. Running the AI in shadow mode for 2–3 days ensures accuracy without disrupting your live system [2].
Once your claim data is connected, the platform quickly analyzes denials and drafts custom appeals.
Automating Denial Analysis and Appeal Creation
After integration, the AI reviews 835 remittance files and clinical records, identifies missing information, and creates tailored appeal letters using payer-specific language [14][16][4]. It employs natural language processing to extract clinical evidence supporting the medical necessity of the denied service [16].
In 2023, a mid-sized medical practice implemented this system and cut denial resolution time from 30 days to just 24 hours, saving $50,000 annually in administrative costs [15]. The AI prioritizes cases based on their likelihood of success and revenue potential, ensuring your team focuses on the most impactful opportunities [16]. Complex or ambiguous cases are escalated to human experts, while the AI efficiently handles repetitive tasks [2]. This automation reduces manual work and streamlines the appeals process.
Monitoring Appeals with Live Updates
Once analysis and appeal creation are automated, ClaimPath keeps track of outcomes to ensure timely resolutions. The platform offers real-time dashboards that show the entire claim lifecycle, including risk levels (Low, Medium, Fixed) and comparisons of received payments against expected contract rates [5][2]. The AI performs 24/7 status checks by logging into payer portals to retrieve updates and interpret remittance data [5][2].
For example, in March 2026, Smilist used ClaimPath to automate high-volume follow-up tasks with real-time monitoring across payer portals, gaining instant visibility without needing complex API integrations [2]. Alerts are sent via Slack, Microsoft Teams, or email, notifying staff only when human intervention is necessary. This constant follow-up helps prevent appeals from lingering in backlogs and ensures they are resolved within required deadlines [17][5].
You can customize the platform to define when a case should be escalated, such as for unclear payer policies or missing medical records [2]. Dashboards also help identify recurring denial patterns, allowing you to address systemic issues and prevent future problems [6]. Always send appeal documentation through certified mail or secure electronic portals to maintain a clear, verifiable paper trail [17]. This continuous monitoring ensures ClaimPath delivers better claim resolution results.
Results from Using ClaimPath
ClaimPath brings measurable improvements to healthcare providers through its automation and precision in handling claim resolutions. By using AI to streamline denial analysis and automate appeals, it’s reshaping how health insurance claims are managed.
Providers and policyholders utilizing ClaimPath report faster resolution times and higher success rates for appeals. For example, ClaimPath’s automation has cut the denial-to-appeal timeline by 75% and significantly increased appeal success rates. Banner Health achieved a 32% success rate on DRG downgrades in October 2025 - an impressive 50% improvement over manual methods - and saw a 20% boost in daily appeal output. Similarly, Legacy Health reported a 55% success rate on overturned appeals and an 89% collection rate with the help of AI-driven processes [20].
AI-generated appeals consistently outperform manual efforts, achieving 25% higher success rates for DRG downgrades and 37% higher success rates for inpatient admission denials [20]. In fact, 70% of insurance appeals succeed when actively pursued [22].
Time and Cost Savings Through Automation
ClaimPath eliminates repetitive administrative tasks, saving significant time and money. For instance, it reduces claim processing times from 6–10 minutes to just 30–55 seconds [21][12]. Even complex reports requiring clinical documentation review are processed in under 3 minutes, compared to the 6 hours needed manually [23]. This efficiency slashes manual administrative work by 90% to 98% [21][12].
One standout example comes from a California medical technology startup, which saved over $90,000 in January 2025 by automating 2,300 hours of manual labor. Within three weeks, ClaimPath’s AI cleared 80% of a 3,000-record denial backlog, reducing per-claim processing time from 6 minutes to just 30 seconds [21]. Other healthcare organizations report saving over 500 hours of manual work each month, allowing staff to focus on more complex cases that require human expertise [21][12].
Performance Data and Examples
The data paints a clear picture of ClaimPath’s impact. AI-powered denial management has led to a 50% reduction in denial rates for affected claims [18]. Organizations using generative AI have reduced initial denial rates from 11.99% to 8.39% by identifying errors before claims are submitted [19]. Additionally, health systems implementing AI agents report a 30% drop in claim denial rates within 90 days of adoption [2].
| Metric | Manual Process | AI-Powered Process |
|---|---|---|
| Processing Time per Claim | 6–10 minutes [21][12] | 30–55 seconds [21][12] |
| Denial to Appeal Timeline | 40 days [20] | Single-digit days [20] |
| Manual Rework | High baseline | 90% eliminated [21] |
| Success Rate (DRG Downgrades) | Traditional baseline | 50% improvement [20] |
| Administrative Costs | Standard baseline | Up to 70% lower [19] |
Beyond time savings, the cost benefits are substantial. Reworking a single claim manually costs providers between $25 and $30, and up to 65% of denied claims are never resubmitted due to the administrative burden [2]. ClaimPath makes it feasible to appeal these abandoned claims, recovering lost revenue. Additionally, organizations using AI for medical coding have saved over $1 million through enhanced accuracy and fewer errors [19].
These results highlight how ClaimPath is revolutionizing denial management and creating new opportunities for healthcare reimbursement advancements.
Conclusion
Health insurance denials cost U.S. healthcare providers an estimated $262 billion annually, with a staggering 86–90% of these denials being preventable [10][24]. When appeals are pursued, providers can achieve success rates of 70% to 80% or even higher [3].
ClaimPath offers a game-changing solution by automating denial management. From detecting errors before submission to generating appeals and following up with payers, it transforms what used to take hours into actions completed in seconds. This automation not only shortens the time needed to draft appeals but also improves the effectiveness of contesting denials [3][7]. Beyond speeding up processes, it helps prevent denials entirely by addressing issues like coding errors, missing documentation, and eligibility problems before claims are filed. Providers using ClaimPath have achieved denial rates as low as 3.1%, far below the industry average [10].
ClaimPath showcases how AI can revolutionize denial management by identifying potential problems early and automating solutions. It integrates seamlessly into existing workflows, requiring no complex API builds or system overhauls. Whether handling thousands of claims or tackling a single challenging denial, ClaimPath scales to meet the needs of any organization. As part of AgentBandwidth's AI-driven tools, it empowers providers to reclaim lost revenue and reduce administrative burdens. The results speak for themselves: organizations adopting AI for denial management report significant improvements in efficiency and financial outcomes within just 90 days [2]. This shift toward automation clearly delivers both operational and financial benefits.
FAQs
What’s the difference between a rejected claim and a denied claim?
A rejected claim is one that never makes it through the initial processing stage by the payer. This usually happens because of errors or missing details in the submission. On the other hand, a denied claim is one that has been fully reviewed but officially declined for payment. Denial comes with specific reasons or denial codes explaining why it was not approved.
To address these issues, rejected claims need to be corrected and resubmitted, while denied claims often require an appeal or additional documentation to challenge the decision.
What documents do I need to win a medical-necessity appeal?
To improve your chances of success in a medical-necessity appeal, start by collecting all relevant documentation that supports the treatment's necessity. Make sure the records align with the insurance provider's coverage criteria and verify that medical coding is accurate. If there are errors, submit a corrected claim to help smooth the process. The key is to provide clear, detailed, and precise records to strengthen your appeal.
How does ClaimPath integrate without building APIs?
ClaimPath utilizes AI agents to handle a range of tasks, including logging into payer portals, interpreting remittance data, initiating appeals, and managing follow-ups until the issue is resolved. These agents function like virtual team members, completing tasks independently without the need for direct system integrations or custom APIs.
